|
8/16/2023 0 Comments Dot blot hemorrhages 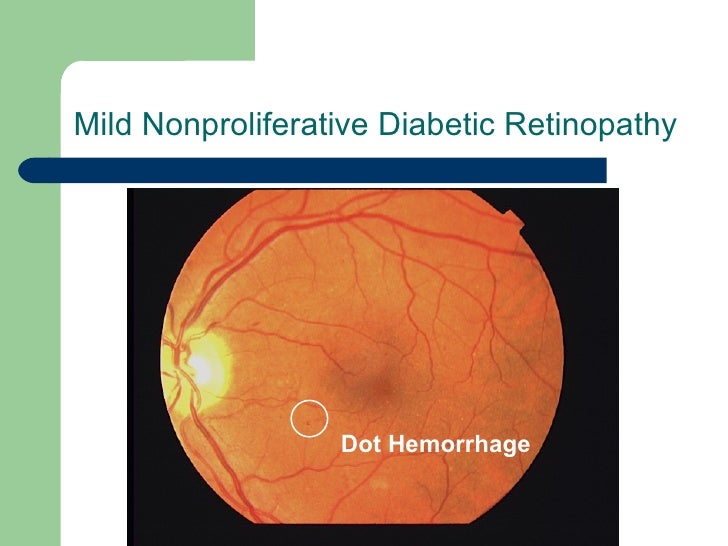
This is an evolving paradigm, however, and many retina surgeons have not yet embraced this approach. 5-8 Though these patients have not yet developed traditionally treatable disease with either macular edema or proliferative changes, there is value in decreasing the level of retinopathy, potentially delaying or preventing the development of sight-threatening complications. 5-8ĭata from anti-VEGF studies such as RISE, RIDE and PANOROMA show patients with moderately severe (or worse) retinopathy have the potential for at least a two-step improvement on the DR Severity Scale (DRSS) when given anti-VEGF drugs such as ranibizumab (Lucentis, Genentech) or aflibercept (Eylea, Regeneron). However, anti-vascular endothelial growth factor (anti-VEGF) injections are now considered primary therapy to improve DR severity. Historically, moderate NPDR was monitored and not treated. These patients are at significantly higher risk for worsening DME. Keep in mind that some patients have subclinical diabetic macular edema (DME), only observable with OCT. OCT may be appropriate to confirm or rule out the presence of macular edema. Fluorescein angiography (FA) may be indicated if VB or IRMA are present. Mild venous beading (VB) and intraretinal microvascular abnormalities (IRMA) are also seen in moderate NPDR. 2 Moderate NPDR will show an increase in intraretinal hemorrhages and microaneurysms, as well as hard exudates and cotton-wool spots. This stage is considered more than just microaneurysms, but less than severe NPDR. While traditional optical coherence tomography (OCT) is not indicated for mild NPDR unless retinal thickening is observed with stereoscopic clinical examination or visual acuity is reduced, OCT angiography (OCT-A) can be a useful tool to detect capillary dropout and small microvascular changes that are not otherwise noted on dilated fundus exam ( Figure 2). Further diagnostic testing is not indicated in mild NPDR, but fundus photography is often helpful to establish a baseline level of retinopathy to assess future progression, and is useful for patient education. This stage is characterized by microaneurysms, dot/blot hemorrhages or hard exudates or a combination of all three. In a sense, this is your most important task as it sets the tone for the management decisions to follow. 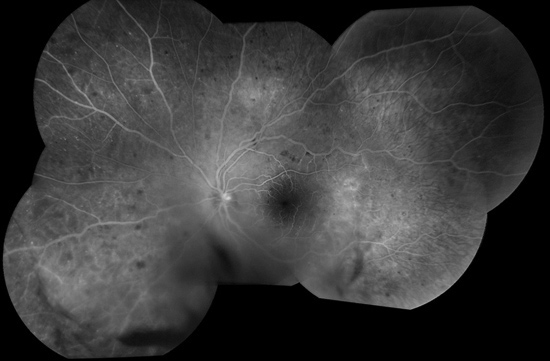
This fundus shot shows a patient with signs of moderately severe NPDR. So, what are the signs for the various stages of DR that allow practitioners to effectively categorize the disease process?įig. PDR can be further categorized into non-high risk and high risk ( Table 1).įinally, with all levels of retinopathy, you should definitively determine the presence or absence of macular edema. NPDR should be labeled as mild, moderate, severe or very severe. Next, classify the DR as either non-proliferative (NPDR) or proliferative (PDR). 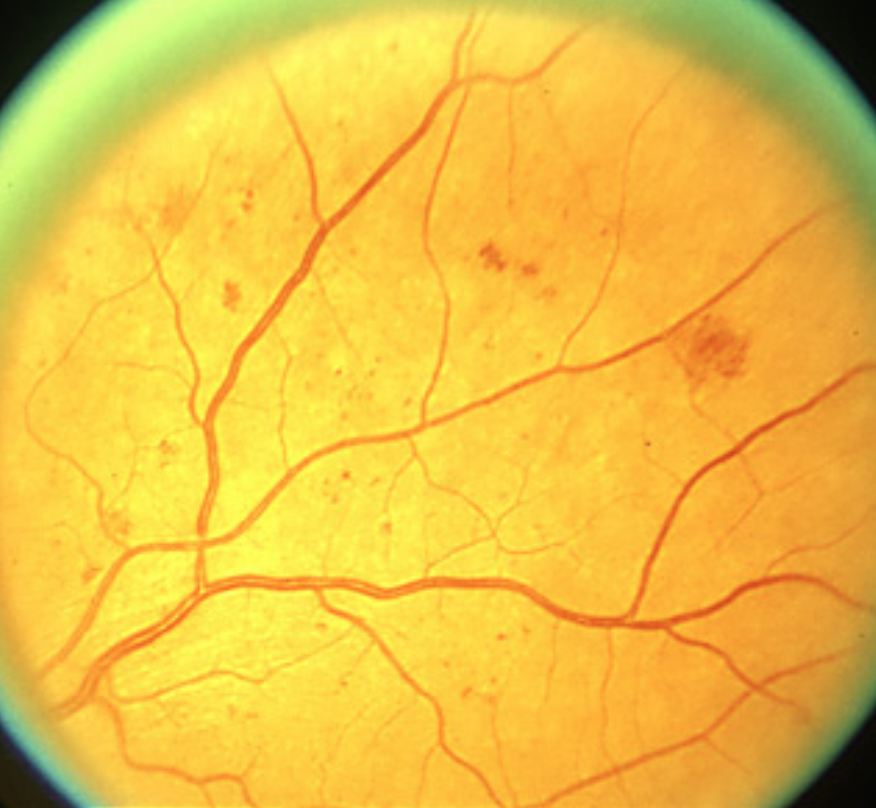
Note the location of any diabetic changes in the fundus. 1-3Īny therapeutic protocol will depend upon staging the severity of the DR. Do you monitor the patient or refer to a retina specialist? The answer can be somewhat tricky because multiple practice guidelines for managing diabetic retinopathy (DR) exist, both from optometry and ophthalmology in the United States, as well as internationally. Now it’s time to determine your next step. You have dilated your diabetic patient and their fundus shows signs of retinopathy ( Figure 1 ). My Patient Has Recurrent Corneal Erosion.Now What? Each installment in the five-part “Now What?” series will cover a different chronic condition: To help optometrists strengthen their protocols for managing conditions that require ongoing-perhaps life-long-care, this series explains the steps to take after confirming a diagnosis, from day one through long-term management. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
